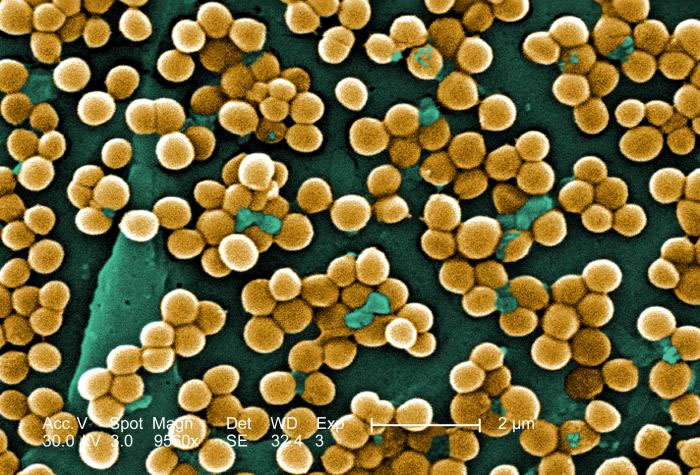
Staphylococcus Aureus (S. aureus) is a common microbe found on the human body. It is usually spread by skin-to-skin contact, and most commonly causes skin eruptions such as boils and styes that can be easily treated with oral and/or topical antibiotics. However, certain strains of S. aureus are capable of structural change, making them resistant to antibiotics. They are, as a result, difficult to eradicate and easy to transmit. Two such strains are MRSA (methicillin-resistant staphylococcus aureus), usually related to hospitals and health care workers (HCWs), and CA-MRSA (community-related MRSA), widespread S. aureus infections originating outside of a hospital setting.
Hands
MRSA and CA-MRSA are most commonly spread by someone who has skin contact (hand-to-hand or hand-to-body) with an infected person and then has contact with another person. Sometimes the carrier is "colonized" with the microbe but has no signs of infection himself. Skin contact is especially threatening if open sores or cuts exist on either the carrier or the receiver. In spite of diligent hand washing, the spread of MRSA in hospital settings can be rampant. This led Ben-David, M.D. et al. to conduct a 2008 study in which they concluded that non-symptomatic HCWs were often colonized and needed to be decolonized to arrest the spread of MRSA.
Inanimate Objects
Live S. aureus are often found on surfaces and fabrics within hospital settings, including sinks, trays, towels, bedding and privacy curtains. The length of time that the organism can survive without a host depends upon the surface itself, but it is typical that a HCW, patient or visitor may handle a contaminated surface and carry the germ to another person. In regard to CA-MRSA, it is recommended that people do not share towels, razors, clothing, personal grooming items, etc., especially if there is a known infection within the family or community.